Resistant bacteria will be more dangerous than cancer in 2050

This column is written by Stig Bengmark – Professor Emeritus, scientist, lecturer and writer. Read more of Stig Bengmark’s columns here.
Just a few decades ago, there was a real euphoria in medical circles. As can be seen from the picture below, severe diseases caused by various infections, e.g. tuberculosis, and sexually transmitted diseases such as syphilis, etc. (all above the red line in the image below), have been combated successfully during the last century.

But things look less hopeful now. Even now, around 50,000 people die each year in the United States and the EU alone from infections for which there is currently no effective treatment. The bacteria that cause these infections have given themselves total dominance by developing complete resistance to the very drugs that not long ago created a medical success the like of which we’d never seen before.
If you compare this with cancer – the world’s most common cause of premature death (in the USA alone, for example, more than 550,000 deaths every year) – today less than 5% die as a result of resistant bacteria. This will not be the case for long – unless a miracle happens. Although the number of deaths from cancer globally is estimated to triple by 2050, as it stands today, mortality from infections caused by resistant strains is estimated to surpass cancer as the leading cause of death on earth by this time. It’s estimated that every year 10 million of the world’s population succumb to untreatable infections, which will incur enormous costs for our societies – $100 trillion in expenses for pointless treatments and lost income from those who die.
The WHO makes clumsy attempts to reduce the consequences
In a desperate attempt to reduce the increase in the number of cases of resistant strains, the WHO has produced a plan which was recently adopted by the 68th General Assembly. Unfortunately, it’s completely lacking any new or radical proposals at all – it just repeats things we already know and which have so far been proved quite ineffective, such as:
- Improve infection prevention in hospitals and health centres
- Prescribe antibiotics only when absolutely necessary
- Never prescribe stronger antibiotics than are truly necessary
According to the report, politicians in the various member states can in particular ensure that:
- The development of resistant strains is better monitored than is the case today
- Prevention of infections and control over their occurrence are given better priority than at present
- The use of medicines, especially antibiotics, be better regulated by law than is the case at present
- The general public be better informed of the problem of antibiotic resistance
- Support and show appreciation for innovation in various ways with a view to creating new initiatives for the prevention and treatment of resistant strains
- Support the development of new diagnostic tools, vaccines, and other new treatment methods to a greater extent than at present
Newly-discovered tribal remnant gives a new perspective
In 2009, a tribal remnant was found in one of the most inaccessible parts of the Amazon, in Venezuela – a group that has most likely not been in contact with any other people since they arrived in South America more than 11,000 years ago. A medical team visited them fairly soon after and conducted extensive medical examinations. They were forward-thinking enough to also take samples of the intestinal flora of this population, called the Yanomami. The intestinal flora has now been examined in detail and a research report has recently been published (Clemente et al. Sci. Adv. 2015;1). Quite surprisingly, these individuals turned out to have an intestinal flora that’s 40% more expansive than any known people, which indicates that large parts of our intestinal flora have become extinct during the civilisation process – perhaps it was a lot of the most important ones for our health?
Among other things, it has come as a great surprise to find that these individuals have no less than thirty bacteria with antibiotic-resistant genes. Perhaps the bacteria of our ancestors, which defended them against various toxins in the environment, had antibiotic properties? Maybe it’s a prerequisite for success with antibiotics that these bacteria have been eradicated? And, if so, is the possible use of antibiotics maybe just an historical interlude?
For millions of years, our own bacterial flora was our only protection against disease
I believe that the treatment we should turn to first is reconditioning the poorly functioning intestinal flora – the addition of pro- and synbiotics is a risk-free and very promising alternative. For more than 30 years, I’ve collaborated with colleagues around the world in an attempt to replace dangerous antibiotics with totally risk-free pro- and synbiotics – declared by the health authorities as GRAS (Generally Regarded As Safe). This has led to a product for gut reconditioning – Synbiotics 2000 – which has been tried with great success on various seriously ill people in intensive care, not least people undergoing transplants, mostly liver but also bone marrow, people who’ve been in severe accidents, etc. and it’s been shown to greatly reduce the incidence of infections. Now it’s also going to be tested on ADHD, acute psychosis, and as a supplement for dialysis treatment.
One young man who underwent a bone marrow transplant and who refused to take antibiotics was the first to try Synbiotic 2000 instead. It’s worth considering that he was treated with live bacteria in a situation where his own immune system was completely snuffed out. There was nothing unusual about the aftermath of his treatment and he went home in record time.
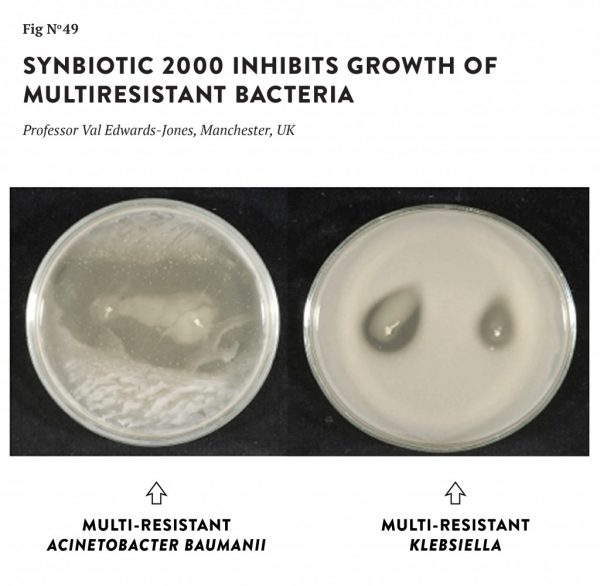
10 years ago, the microbiologist and professor Val Edward-Jones, Head of Research Development at the University of Manchester, helped me to look at Synbiotic’s effect on resistant bacteria in the laboratory, which she described as comprehensive (see photo).
A standard course of antibiotics destroys 90% of the gut flora
It’s frightening information that our most used and appreciated drugs – antibiotics – actually contribute to the development of serious diseases that are so rapidly increasing in the west and all over the world: allergies, often asthma and skin eczema, but also obesity, diabetes, Alzheimer’s, and various types of cancer.
So far, it’s hardly been taken into account that modern humans’ already severely diluted flora of intestinal bacteria (perhaps in contrast with that of our ancestors) has a poor tolerance towards the presence of chemicals, and of course, especially those that are made to destroy bacteria such as antibiotics. It’s actually been calculated that an ordinary course of antibiotics on average destroys 90% of the intestinal flora (microbiota) and, thereby, immune functions, bile metabolism, and the production of important hormones such as prostaglandins and steroids (Caetano L et al. Antimicrob Agents Chemother. 2011;55:1494-1503) – and it often takes years before the gut flora and gut function are back to normal.
Unfortunately, cancer drugs have the same effects – chemotherapy drugs reduce the intestinal flora by about 100 times, and the particularly sensitive aerobic bacteria by about 10,000 times (they’re completely eliminated). In addition, the intestinal content of more resistant malignant and pathogenic bacteria, often called Gram-negative bacteria, increases about 100-fold (Van Vliet MJ et al. Clin Infect Dis 2009;49:262-270). Even common and daily-use medications such as blood pressure and sleeping medications leave their miserable traces in the gut flora. A fairly recently published study (Nonzee V et al J Med Assoc Thai 2012; 95: 96-104) shows that common blood pressure medications cause dysbiosis (a poorly functioning intestinal flora) but that it also reduces the production of the important membrane-protecting mucus layer.
Always be careful with medicines – they always drag down your immune system
Ordinary gastric ulcer medicines that you buy without a prescription at the pharmacy also affect the intestinal flora – if they’re used during pregnancy, for example, they significantly increase the foetus’ risk of developing asthma later in life (Andersen AB et al. Aliment Pharmacol Ther 2012;35:1190-1198). Recently published studies from India show that if a diarrhoea patient, for example, is treated with antibiotics, the individual’s resistance is significantly reduced and the time until the next diarrhoea episode is significantly shortened (Rogawski ET et al Int J Epidemiol. 2015 E-pub). Another recently published study (Boursi B et al Eur J Endocrinol 2015; 172: 639–648) shows that for every course of antibiotics an individual undergoes, the risk of later developing diabetes increases significantly: 2-5 courses in life by 8% (if quinolones 15%) and more than 5 courses in life by 23% (if quinolones 37%). Another study shows that if you take up to 18 sleeping pills per year, the risk of premature death increases by 3.6 times, between 18 and 132 sleeping pills per year, it increases by 4.4 times, and with more than 132 tablets per year then by no less than 5.3 times (Kripke DF et al BMJ Open 2012: 2).
The favourite food of bacteria – plant fibre
Our biggest health dilemma is that we’ve stopped eating the amount and the type of food that our protective bacteria want. It needs to be told like it is – this is what is making us so sick – and it’s predicted to get worse. It’s about fibres, I repeat, fibres.
In my article on fibre, I discussed the importance of plant fibre for our protective bacteria’s survival and growth over time. This is also why I’ve given my probiotics 10 grams of fibre – 2.5 grams each of four different varieties: beta-glucans, inulin, pectin and resistant starch. Ideally, I’d like to add a lot more, but I have to content myself with pointing out the importance of the consumer eating lots and lots of fibre. The effect is what you make it.
I pointed out things such as the National Food Administration of various western countries recommending an intake of fibre of 25-35 grams per day, which I think is far too little. But the truth is that people in the United States and Western Europe, for example, currently only eat half as much – 15-20 grams – which is a disaster. Keep in mind that the people who have the best intestinal flora on earth consume plants equivalent to upwards of 150 grams of pure fibre every day.
Honour your gut bacteria and you may thrive and survive on this planet for a long time
Two overriding rules for optimal health apply:
- Satisfy your health bacteria’s need for large amounts of fibre every day
- Reduce/exclude all toxins, both those that the toxic bacteria in the body creates as endotoxins, and those that are brought in from outside, everything from chemicals to medicines.
Then there are some rules – my twelve commandments.


